
Patient-level data not available, only summaries at the nursing home level. Risk-adjusted composite measures for quality outcomes allow for meaningful comparisons.Ĭomparisons can be made on national/state/facility level for different time periods. Observational assessment and medical records review of patients (MDS data)ĭata includes all Medicare and Medicaid-certified nursing homes and are ideal for doing research on regional and state variation on quality outcomes.ĭata can be linked with other CMS datasets. Inspection reports / observational assessment Number of Nursing homes varies year to year Hospitals and health care facilities/providers, All Medicare and Medicaid-certified nursing homesġ5,652 (January 2017) Medicare and Medicaid participating nursing homes included Health and fire inspection deficiencies at nursing homes, staffing numbers per resident and association with quality care, short and long stay outcomes. 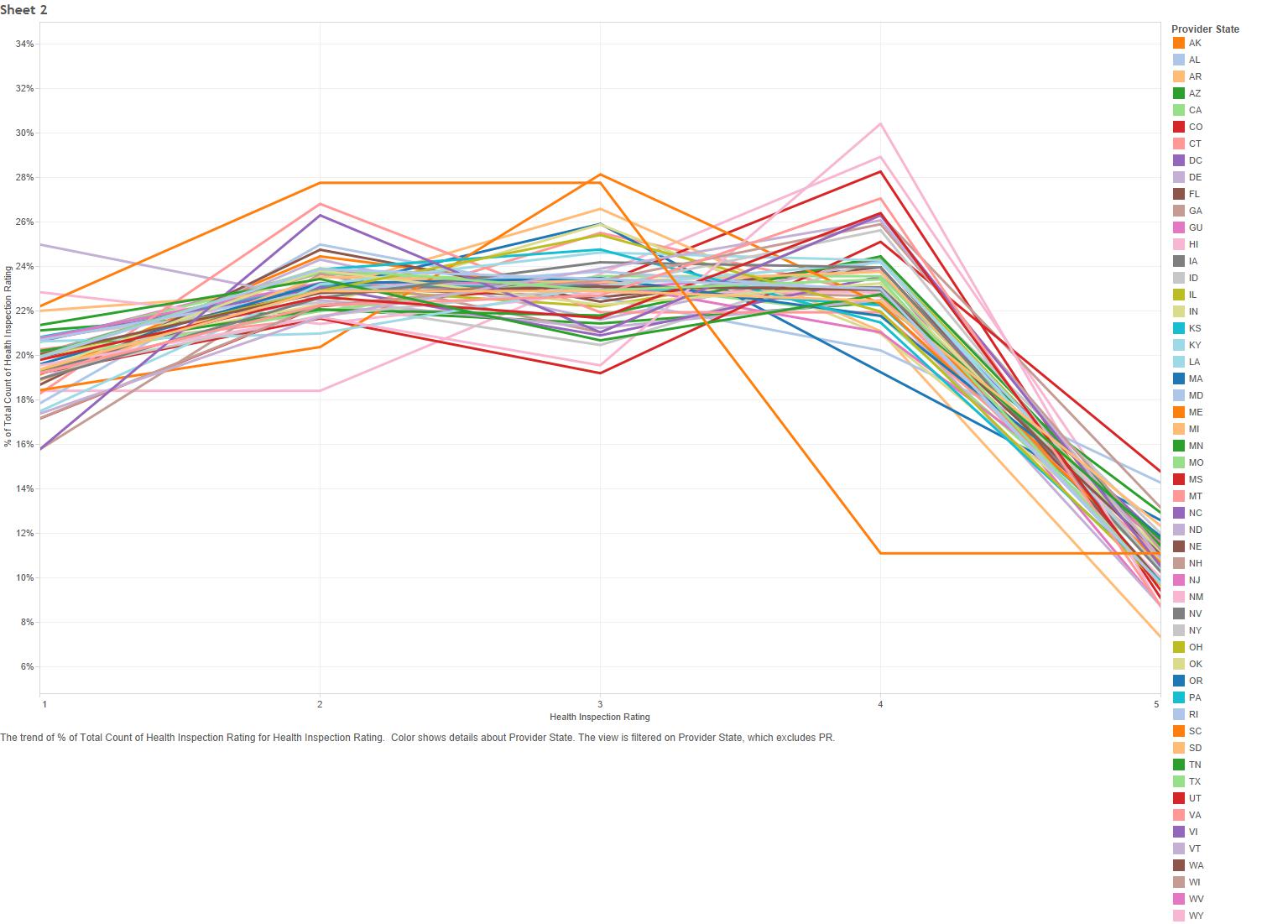
Long-stay residents measures: Proportion reporting: Falls, urinary tract infections, moderate to severe pain, pressure ulcers, functional status independence/improvement, weight loss, need for help with daily activities increased, depressive symptoms Short-stay resident measures: Proportion with: Functional status, hospital readmissions, emergency room visits, discharge to community, new or worsened pressure ulcers. Longitudinal assessment of nursing homes’ improvement in quality outcomes State and regional variations in nursing home quality outcomes. Skilled Nursing care, swing beds, nursing home quality of care, nursing home staffing information, regulatory compliance, long-stay quality outcomes, short-stay quality outcomes, MDS datasetĬenters for Medicare & Medicaid Services (CMS), Department of Health and Human Services (HHS) All data is aggregated at the national, state and individual Nursing Home level. Note that no patient level data is available. The Nursing Home Compare uses a “five star rating” system, which is a composite measure derived from health inspection findings of these facilities, staffing (e.g., availability of nursing staff per resident per day), and quality measures (e.g., falls, pain, functional status, hospital readmissions). This ongoing data collection aims to assist consumers (including patients) in selecting nursing homes by evaluating outcomes and deficiencies. The Centers for Medicare and Medicaid Services (CMS) launched a quality rating system for Medicare and Medicaid certified nursing homes (skilled nursing and long-term care facilities) on December 2008. Rehabilitation Dataset Directory: Dataset Profile Dataset: Nursing Home Compare () Basic Information Staffing data are submitted by the facility and are adjusted for the needs of the nursing home residents.įor more in-depth information of the Five-Star Quality Rating System, please read the Technical Users' Guide.Rehabilitation Dataset Directory: Search / Total staffing includes RNs, licensed practical nurses or licensed vocational nurses, and certified nurse aids. Staffing rating is based on two measures: the number of registered nurse (RN) hours per resident day and the total staffing hours per resident day.QMs are derived from clinical data reported by the nursing home. Quality Measures (QM) rating combines the values on nine QMs (a subset of the 19 QMs listed on Nursing Home Compare) to create the QM rating.We place more emphasis on recent inspections. Health Inspections rating is based on the three most recent comprehensive (annual) inspections, and inspections due to complaints in the last three years.If a nursing home is a Special Focus Facility, the maximum "Overall" rating is three stars.If the "Health Inspections" rating is one star, then the "Overall" rating cannot be upgraded by more than one star based on the "Staffing" and "Quality Measure" ratings.Add one star if the "Quality Measures" rating is five stars subtract one star if the "Quality Measures" rating is one star.Subtract one star if the "Staffing" rating is one star. Add 1 star if the "Staffing" rating is four or five stars and greater than the Health Inspections Rating.Start with the Health Inspections Rating. 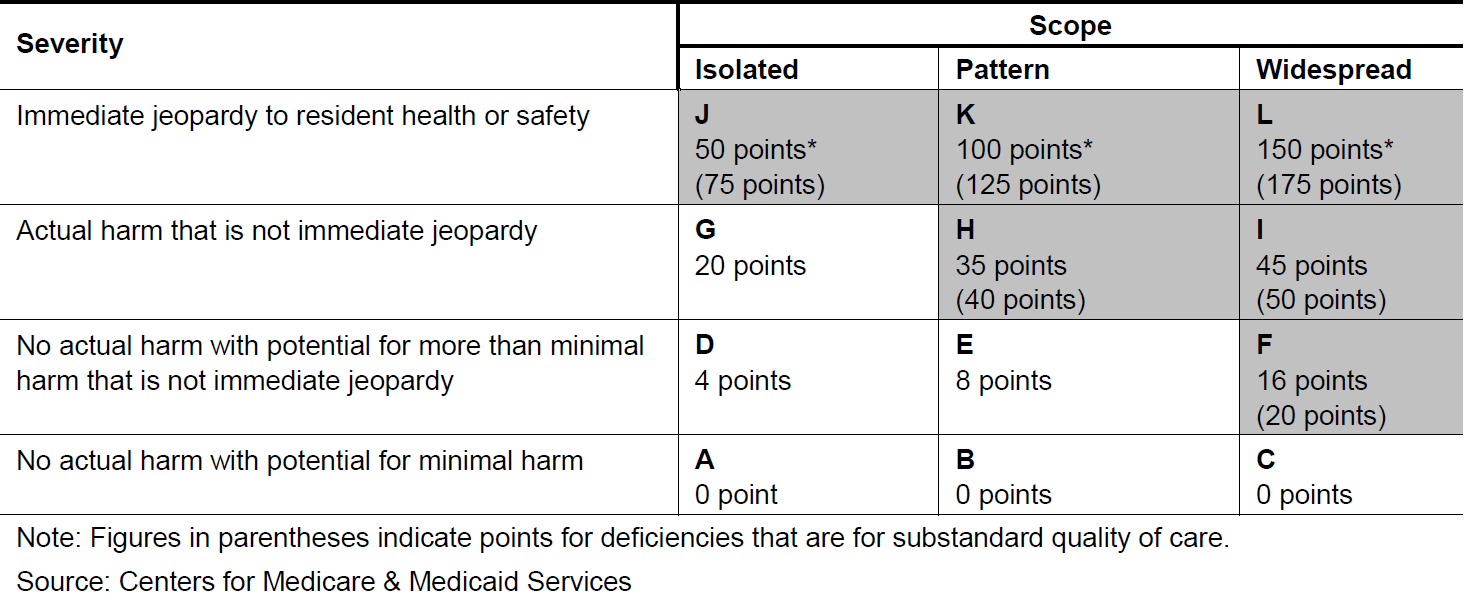
How CMS calculates ratingsĬMS assigns the Overall Five-Star rating using the following steps: 
Each facility is rated from a low of one star to a high of five stars based on three critical areas: health inspection results, quality measures and staffing levels. Nursing Home Compare, which is managed by the Centers for Medicare and Medicaid Services (CMS), provides quality ratings for each of the nation's approximately 16,000 Medicare and/or Medicaid-certified nursing homes.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
